Products
Services
October 19, 2016
Since CMS’ release of the final rule for the Medicare Access and CHIP Reauthorization Act (MACRA) last Friday, October 14, 2016, we have been reviewing the final proposal of the Quality Payment Program (QPP). From that review, we have found that CMS has made participation for 2017 under the QPP easier than the previous Meaningful Use, PQRS and VM programs, which are now combined under the MACRA legislation.
Since Meaningful Use Stage 1, ChartLogic has been able to maintain its readiness with each new stage and program. The MACRA legislation is no different and we are able to meet any level of participation of the new QPP in which our physician practices choose to participate.
With the majority of the Merit-Based Incentive Payment System (MIPS) score being focused on the Quality Category with Advancing Care Information Categories, ChartLogic will be able to continue to meet and exceed the requirements for these two categories. The categories and measures mentioned are the same for practices who have successfully attested in for MU Stage 1 and/or Stage 2 and can easily be met by continuing to use the system as designed. We will also have our Meaningful Use Consultants ready to help navigate the reporting requirements as we progress into 2017.
The Quality Payment Program has simplified previous programs in the following ways:
The lighter requirements for the 2017 performance year places ChartLogic and its customers in the best possible situation without having to make major upgrades to existing software, thus allowing a smoother transition to the MACRA legislation. Practices who had not participated in the Meaningful Use program due to is complexity will now be able to participate in the new Quality Payment Program due to its greater flexibility.
“All of our customers are in an excellent position. ChartLogic is ready to help them meet MACRA requirements at the pace or timeline that works for them. Our current version has everything available for them to be successful with no software update necessary.”
– Chris Langehaug SVP of Operations, ChartLogic
The final rule for the for MACRA is in an attempt to streamline Medicare payments. The Quality Payment Program is focused on moving from the fee-for-service payment system to one that rewards quality, patient-centered care.
MACRA will reform Medicare payments for more than 600,000 clinicians across the country. To know if you are part of this group, you must bill Medicare more than $30,000 a year or provide care for more than 100 Medicare patients a year, and are one of the following:
There are two tracks from which you can choose how you want to participate in the Quality Payment Program based on your practice size, specialty, location, or patient population. The first track is the Merit-Based Incentive Payment System (MIPS) and the second track is the Advanced Alternative Payment Models (APMs). For more details, view our previous blog post: Deciphering the Confusion of MACRA, MIPS & APM.
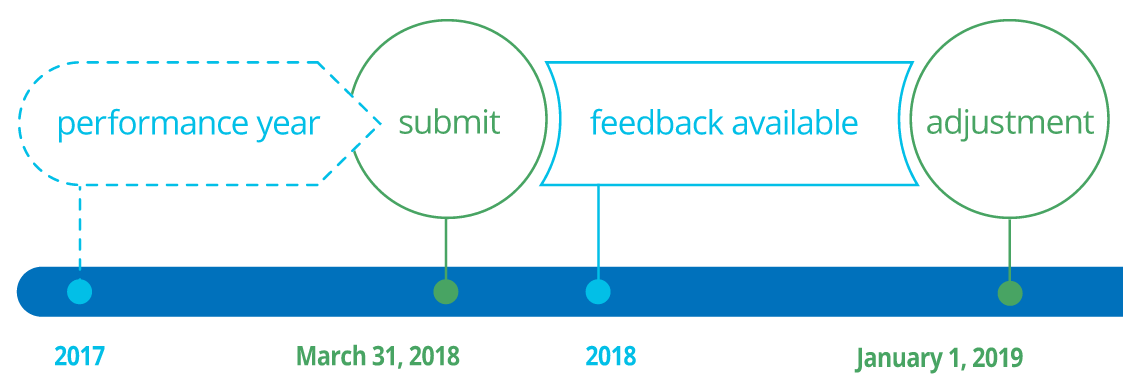 Source: CMS Quality Payment Program Website
Source: CMS Quality Payment Program Website
Performance: The first performance period opens January 1, 2017 and closes December 31, 2017. During 2017, you will record quality data and how you used technology to support your practice. If an Advanced APM fits your practice, then you can provide care during the year through that model.
Send in performance data: To potentially earn a positive payment adjustment under MIPS, send in data about the care you provided and how your practice used technology in 2017 to MIPS by the deadline, March 31, 2018. In order to earn the 5% incentive payment for participating in an Advanced APM, just send quality data through your Advanced APM.
Feedback: Medicare gives you feedback about your performance after you send your data.
Payment: You may earn a positive MIPS payment adjustment beginning January 1, 2019 if you submit 2017 data by March 31, 2018. If you participate in an Advanced APM in 2017, then you could earn 5% incentive payment in 2019.